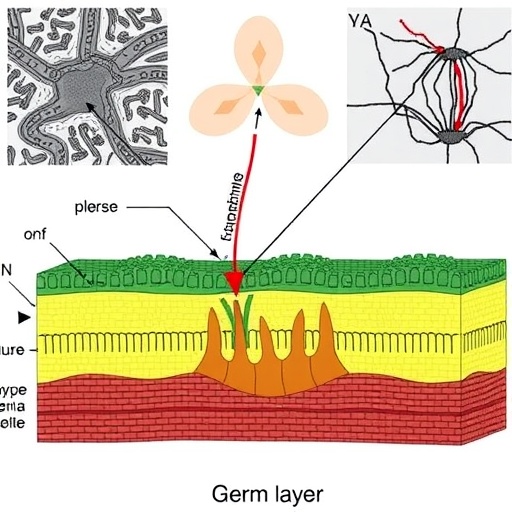
Recent advancements in lymphoma research reveal groundbreaking insights into the patterns of extranodal invasion driven by the germ-layer origins of affected organs. Investigations focused on diffuse large B-cell lymphoma (DLBCL), a heterogeneous and aggressive cancer subtype, have identified a striking organotropism that aligns closely with embryological development. This novel perspective offers a fresh understanding of lymphoma dissemination and reveals critical molecular and cellular underpinnings that could reshape therapeutic strategies.
Patients with DLBCL involving extranodal sites were categorized according to the germ-layer origin of the invaded tissues—ectoderm, endoderm, or mesoderm—allowing researchers to unravel complex biological variations underlying these distinctive disease phenotypes. The ectodermal group included organs such as the central nervous system, skin, breast, and nasal cavity. Endodermal involvement encompassed the gastrointestinal tract, thyroid, liver, lung, and pancreas, while mesodermal invasion was observed in bone, bone marrow, testes, kidneys, adrenal glands, and reproductive organs. Patients whose lymphoma was confined to lymph nodes constituted the control arm of the study.
Following standard R-CHOP chemotherapy, survival analyses uncovered a profound disparity: the mesodermal group consistently exhibited inferior progression-free and overall survival compared to both ectodermal and endodermal groups. This clinical divergence prompted deeper molecular investigations, which revealed unique mutational landscapes tailored to the organ-specific germ-layer contexts. Ectodermal-extranodal lymphomas were enriched for mutations in MYD88, PIM1, and TBL1XR1, while endodermal sites bore mutations predominantly in TP53 and TET2. The mesodermal infiltrates combined mutations seen in ectodermal groups with additional CD79B alterations, defining a complex mutational signature tightly coupled with poorer outcomes.
Harnessing advanced gene-editing technologies, researchers modeled these mutation profiles within lymphoma cell lines to experimentally validate their roles in organ-targeted migration, or organotropism. Using zebrafish xenotransplantation models—an emerging platform for studying cancer dissemination—the distinct mutational combinations dictated directional migration toward representative organs of each germ layer. MYD88/PIM1/TBL1XR1 mutated cells demonstrated rapid migration to the brain and hematopoietic tail tissues, emblematic of ectodermal and mesodermal niches, while CD79B-mutant cells predominantly localized to mesodermal sites. Conversely, TP53 and TET2 mutations precisely drove homing to liver and gastrointestinal organs, epitomizing endodermal tropism. These dynamic migratory patterns poignantly recapitulated developmental cues intrinsic to their germ-layer origins.
Strikingly, the temporal sequence of lymphoma cell dissemination mirrored the ontogenetic timelines of germ-layer development. In zebrafish models, lymphoma cells manifested early brain migration within two days post-injection, aligning with ectodermal maturation phases. This was followed by subsequent infiltration of endodermal organs such as the liver and gastrointestinal tract by day four, with mesodermal hematopoietic tail tissue involvement occurring last. Single-cell transcriptomic analyses complemented these observations by revealing malignant B cells evolved along trajectories that parallel germ-layer differentiation. These trajectories bifurcated into two distinct fates: one pathway heightened B-cell receptor signaling, while the other maintained persistent T-cell activation signaling, underscoring heterogeneity within lymphoma evolution tied to developmental lineage.
Intriguingly, T-cell populations within the tumor microenvironment did not adhere to this germ-layer developmental timing. In the mesodermal group, CD4+ and CD8+ T cells were predominantly naïve and undifferentiated, characterized by arrested activation states and an immune milieu favoring tolerance. Contrastingly, ectodermal lymphomas were associated with effector and proliferative T-cell phenotypes, such as proliferating CD8+ T cells and follicular helper CD4+ T cells, exhibiting robust activation, cytotoxicity, and antigen presentation. Endodermal environments fostered immune exhaustion and regulatory T-cell expansion, manifesting as immune suppressive landscapes. These findings highlight that the immune microenvironment’s functional states were shaped more by local organ-specific factors rather than embryonic developmental programs.
Differential expression of immune checkpoint molecules further delineated these germ-layer-dependent phenotypes. LGALS9 was predominantly observed in ectodermal sites, PD-L1 was enriched in endodermal tissues, and B7-H3 was specific to mesodermal locations. Functional in vitro assays demonstrated that LGALS9 and PD-L1 enhanced effector T-cell activation and maintained tumor sensitivity to rituximab, a frontline monoclonal antibody therapy for B-cell lymphomas, significantly decreasing tumor cell viability. Conversely, elevated B7-H3 expression incapacitated T cells, maintaining their naïve phenotype and inducing resistance to rituximab. Importantly, silencing B7-H3 reversed immune evasion states and resensitized tumor cells to therapeutic agents, underscoring its role as a promising immunotherapeutic target.
This research constitutes the first robust evidence that lymphoma extranodal infiltration follows a germ-layer-dependent organotropism, an insight that breaks new ground in our understanding of cancer metastasis and invasion biology. The distinct oncogenic mutations, temporally orchestrated migratory behaviors, and developmental trajectory recapitulations together form a paradigm that connects embryology with oncology, potentially providing a predictive framework for disease progression based on developmental lineage signatures.
The implications of this study resonate across translational oncology, emphasizing that therapeutic strategies must be tailored to the germ-layer origins of lymphoma invasion. Precision medicine approaches could leverage these molecular distinctions to optimize immunotherapy, chemotherapeutic regimens, and targeted interventions. The identification of B7-H3 as a mediator of immune escape and therapy resistance particularly opens avenues for novel drug development and combinational therapy with existing treatments such as rituximab.
Ultimately, this pioneering work charts a transformative course for lymphoma research and treatment. By embedding tumor biology within a developmental context, it allows clinicians and researchers to reimagine cancer infiltration as a developmental process hijacked by malignancy. This evolutionary perspective not only advances academic understanding but also holds profound promise for improving prognosis and clinical outcomes through refined, biologically-informed interventions.
The convergence of developmental biology, genomics, and immunology in this investigation exemplifies the future of cancer research—where molecular taxonomy informed by embryological principles guides clinical decision-making. As the oncology community continues to grapple with intratumoral heterogeneity and treatment resistance, such integrative frameworks will be indispensable, elevating personalized medicine from concept to clinical reality.
Subject of Research: Diffuse Large B-Cell Lymphoma Extranodal Invasion and Germ-Layer-Dependent Organotropism
Article Title: Germ-Layer-Dependent Molecular and Cellular Determinants of Lymphoma Extranodal Invasion
Web References: http://dx.doi.org/10.1016/j.scib.2026.03.009
Image Credits: ©Science China Press
Keywords: diffuse large B-cell lymphoma, extranodal invasion, organotropism, germ layers, oncogenic mutations, MYD88, PIM1, TBL1XR1, TP53, TET2, CD79B, tumor microenvironment, immune checkpoint, rituximab resistance, developmental biology