In 2025, the landscape of Medicare Part D prescription drug coverage is undergoing a fundamental transformation that is poised to reshape out-of-pocket expenses for millions of beneficiaries. The enactment of the Inflation Reduction Act (IRA) sought to make prescription medications more affordable by instituting new protections, including a $2,000 annual out-of-pocket cap and the elimination of the notorious “coverage gap.” Yet, a recent white paper authored by researchers at the USC Schaeffer Center for Health Policy & Economics exposes an unsettling paradox: while the IRA provides critical safeguards for high-spending beneficiaries, the majority of Medicare recipients may encounter increased financial burdens due to shifting plan designs and evolving cost-sharing mechanisms.
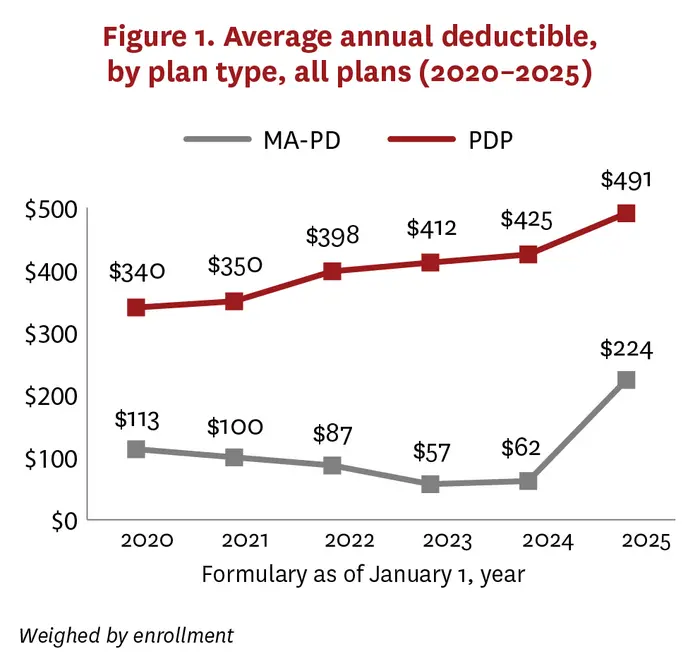
At the heart of this trend lies a striking increase in annual deductibles among Medicare Advantage drug plans. Data reveals that the average annual deductible nearly quadrupled—from $62 in 2024 to $224 in 2025—a sharp reversal of previously stable or modest upward trends. This increase is largely attributable to a precipitous decline in enrollment in “enhanced” plans that traditionally offered zero deductibles. Enrollment in these more generous plans fell from 78% to 41%, signifying a concerted move towards higher upfront costs for beneficiaries before insurance coverage activates.
Stand-alone Medicare Part D drug plans, which operate independently of comprehensive Medicare Advantage offerings, also experienced the largest annual deductible increase on record, with averages rising from $425 to $491. This shift compounds the financial strain on countless beneficiaries, many of whom rely on steady access to critical medications but now face higher entry-point costs before benefits apply. Such steep deductible increases can delay initiation of necessary drug therapies, ultimately leading to adverse health outcomes.
The nature of cost-sharing for commonly used brand-name drugs is evolving just as dramatically. Previously, beneficiaries often paid fixed co-pays for medications, providing predictability and budget stability. However, there has been a pronounced shift towards coinsurance models, in which patients are responsible for paying a percentage of a drug’s list price. This shift is especially pronounced in stand-alone drug plans, where 84.1% of enrollments now require coinsurance, up from just 9.9% in 2020. Medicare Advantage drug plans witnessed coinsurance enrollment rise from 2.6% to 27.5% within a single year, underscoring a sweeping industry-wide pivot.
This reliance on coinsurance exposes beneficiaries to the volatility of drug list prices, which are often artificially inflated through complex rebate and discount arrangements negotiated behind closed doors by pharmacy benefit managers (PBMs). These intermediaries aggressively negotiate secret rebates with drug manufacturers, but crucially, the savings generated are seldom passed directly to patients at the pharmacy counter. Instead, beneficiaries pay their coinsurance based on inflated list prices, resulting in significantly higher out-of-pocket costs compared to traditional fixed co-pays.
The implications of this dynamic are particularly dire for patients taking high-utilization brand-name drugs such as Eliquis, a widely prescribed blood thinner, or Ozempic, a treatment for type 2 diabetes. Both medications command high list prices, and under coinsurance schemes, patients bear an increasing share of these escalating costs. Despite the IRA’s intent to curtail drug spending burdens, this underlying pricing structure fundamentally limits the financial relief that many beneficiaries will experience.
Researchers anticipate some reprieve starting in 2026 when Medicare negotiations under the IRA begin to set drug prices for certain high-cost medications. However, the expanded use of coinsurance diminishes the potential benefits of these negotiated price reductions. Even if list prices fall, beneficiaries paying a percentage of the remaining cost may still face considerable expenses, potentially exceeding what they would have paid under flat co-pay systems. This highlights a persistent flaw: limiting beneficiaries’ protection to an out-of-pocket cap does not inherently solve the problem of inflated drug prices and the indirect cost-shifting mechanisms embedded in the system.
The study’s lead author, Dr. Erin Trish, co-director of the USC Schaeffer Center, emphasizes that the interplay between policy reform and insurance plan design has created a complex tradeoff. While only a small subset of beneficiaries with exorbitant drug spending will benefit directly from the out-of-pocket cap, the majority—those who do not reach the threshold—are likely to face higher medication costs, precipitated by elevated deductibles and increased coinsurance requirements. This situation underscores the need for more transparent, patient-centered reforms in drug pricing and insurance structuring.
A major contributor to this cost burden imbalance is the role of pharmacy middlemen. PBMs, operating largely without transparency, negotiate rebates that lower plan sponsors’ drug expenditures but do not correspondingly reduce beneficiary costs at the point of purchase. Consequently, patients shoulder increasing portions of drug list prices, a structural deficiency that policy changes like the IRA do not fully address. The researchers argue that redirecting rebates directly to patients, rather than plans or PBMs, could substantially alleviate the financial strain on Medicare beneficiaries and enhance medication adherence.
Moreover, this shift in cost-sharing strategies raises critical concerns about access and equity. As deductibles rise and coinsurance replaces fixed payments, beneficiaries with limited financial means or chronic conditions that require expensive medications may delay or forgo treatment, exacerbating health disparities. The phenomenon of medical nonadherence due to cost is well-documented and represents a regressive pressure on vulnerable populations that policy efforts must urgently confront.
The USC Schaeffer Center white paper serves as a timely and incisive analysis of how legislative intent and market dynamics collide in the Medicare Part D arena. It highlights that singular policy levers, such as out-of-pocket limits, are insufficient without concurrent reforms addressing underlying drug pricing structures and plan design incentives. The research calls for comprehensive strategies encompassing greater rebate transparency, alternative cost-sharing frameworks prioritizing predictable patient payments, and strengthened regulatory oversight to curtail PBM practices that distort true drug costs.
As the U.S. healthcare system grapples with perennial challenges of rising pharmaceutical prices and insurance complexity, these findings illuminate an important paradox: well-intentioned reforms like the IRA can inadvertently precipitate higher out-of-pocket expenses for many beneficiaries unless harmonized with systemic pricing and benefit redesigns. Moving forward, policymakers, insurers, and stakeholders must engage in coordinated efforts to identify patient-centric solutions that reduce financial toxicity without compromising access or coverage quality.
The arduous interplay between federally mandated caps, insurance plan reconfigurations, and opaque rebate flows reveals that Medicare Part D reform remains an unfinished endeavor. Continuous monitoring, rigorous evaluation, and innovative policy experimentation will be essential to ensure that the promise of affordable prescription drugs does not become an elusive goal for most Medicare recipients. The USC Schaeffer Center’s research thus provides an urgent call to action, emphasizing the inseparability of drug pricing reform from sensible insurance design in pursuit of equitable, sustainable pharmaceutical access.
Article Title: Shifting Cost-Sharing Burden to Beneficiaries in Medicare Part D
News Publication Date: 19-Jun-2025
Web References: https://schaeffer.usc.edu/research/cost-sharing-burden-medicare-part-d/, https://schaeffer.usc.edu/research/medicare-drug-costs-coinsurance-pbms-jama/
Image Credits: USC Schaeffer Center
Keywords: Health care costs, Health care policy, Drug costs, Health insurance, Medical economics, Health care industry