Hypertension, commonly known as high blood pressure, remains one of the most pervasive chronic conditions affecting nearly half of the adult population in the United States. This stealthy ailment significantly increases the risk of heart attacks and strokes—the leading causes of mortality nationwide. Despite its prominence and the well-documented links to severe cardiovascular complications, public understanding of hypertension’s clinical parameters and manifestations remains strikingly limited. A recent comprehensive health survey by the Annenberg Public Policy Center (APPC) in April 2025 illuminates these gaps in knowledge, revealing a widespread misapprehension regarding what constitutes high blood pressure and the subtle nature of its symptoms.
Clinically, blood pressure is measured as two numerical values representing systolic and diastolic pressures. The systolic number indicates the arterial pressure during cardiac contraction, while the diastolic value reflects pressure during cardiac relaxation. Since 2017, authoritative guidelines from the American Heart Association (AHA) and the American College of Cardiology (ACC) have reset the diagnostic threshold for hypertension at a systolic/diastolic reading of 130/80 mm Hg or higher, lowering the earlier cutoff of 140/90 mm Hg. Despite this recalibration, only a fraction of Americans—approximately 13 percent—can accurately identify these contemporary criteria, underscoring a critical disconnect between medical standards and public perception.
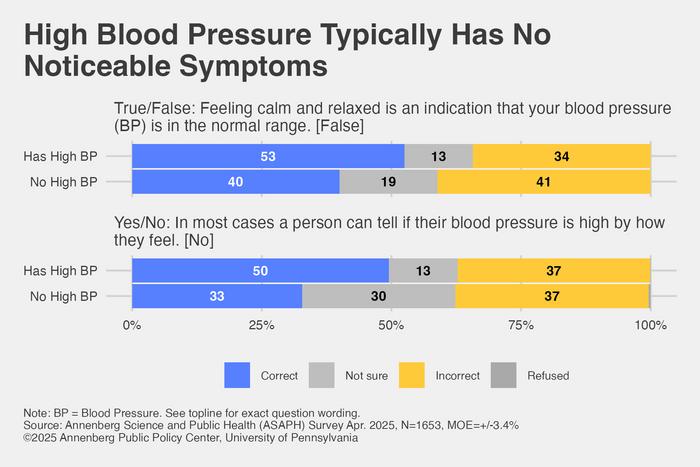
The APPC survey, engaging over 1,600 U.S. adults, underscores several notable misconceptions. More than one-third of respondents falsely believe that high blood pressure is accompanied almost invariably by overt symptoms such as dizziness or shortness of breath. However, hypertension is characteristically asymptomatic, earning it the ominous moniker “the silent killer.” The Centers for Disease Control and Prevention (CDC) corroborate this, noting that most individuals with high blood pressure remain unaware of their condition until adverse cardiovascular events ensue. This survey finding highlights the crucial necessity of routine monitoring, irrespective of subjective feelings of wellness.
Adding to the confusion, nearly 40 percent of participants mistakenly associate a state of feeling calm and relaxed with a normal blood pressure reading. This erroneous belief detracts from scientifically validated methods to assess hypertension and may deter individuals from seeking appropriate evaluation or treatment. Conversely, a robust majority recognize the hereditary component of hypertension, understanding that familial predisposition does not preclude effective management through lifestyle modifications and medical interventions.
Importantly, while fundamental knowledge about what negatively and positively influences blood pressure is relatively widespread, this awareness does not entirely translate into actionable behavior. Most surveyed individuals report familiarity with evidence-based strategies to control high blood pressure, such as maintaining a healthy weight, engaging in regular physical activity, adopting a nutritious diet, managing sodium intake, and adhering to prescribed pharmacotherapy. Yet a measurable gap persists between the intention to engage in these healthful behaviors and their consistent implementation.
The survey sheds light on this dichotomy, revealing that although over 90 percent of respondents assert they would comply with medical advice to watch their diet and monitor sodium intake, only 57 to 72 percent report actually enacting these measures with desired regularity. These data suggest that barriers beyond knowledge—such as motivation, environmental factors, or resource access—may undermine the translation of awareness into consistent health practices. Addressing these barriers could significantly improve hypertension control at the population level.
Regarding pharmacological management, the survey found a high rate of acceptance among those diagnosed with hypertension. Approximately 93 percent indicate willingness to initiate or continue medication when recommended by their healthcare providers. This commitment is consistent with self-reported adherence rates, where 90 percent of patients prescribed antihypertensive drugs claim daily compliance. However, non-adherence in the remaining minority often stems from misconceptions about medication necessity, illustrating the ongoing need for patient education and reinforcement.
Self-monitoring of blood pressure at home is another area of moderate engagement. Approximately 87 percent of respondents express readiness to regularly check their blood pressure if advised by a physician. Yet real-world behavior varies substantially; only 10 percent of hypertensive individuals report daily or near-daily monitoring, while others test less frequently. Health authorities advocate for consistent readings at the same time each day to better inform treatment decisions and mitigate risk, emphasizing the role of sustained patient involvement in disease management.
While there is general parity between individuals with and without diagnosed hypertension in reported health behaviors such as diet and exercise, a notable divergence appears in salt intake. Those aware of their hypertensive status are significantly more likely to limit dietary sodium multiple times per week than their normotensive counterparts. This suggests that diagnosis acts as a catalyst for adopting specific preventative measures, highlighting the critical importance of screening and early detection.
The accumulated data signal both promising and challenging elements within public health efforts to combat hypertension. On one hand, broad awareness exists about lifestyle factors influencing blood pressure, and many express willingness to engage in recommended interventions. On the other hand, persistent misconceptions about the clinical definition and symptomatology of high blood pressure, coupled with incomplete adherence to protective behaviors, represent ongoing obstacles.
Cardiovascular disease prevention strategies must therefore integrate more intensive educational initiatives aimed at demystifying hypertension’s silent nature and clarifying diagnostic criteria. Public health campaigns would benefit from emphasizing routine blood pressure measurement, proper home monitoring techniques, and the value of medication adherence. Ultimately, bridging the gap between knowledge and practice is essential to reducing the morbidity and mortality associated with this pervasive condition.
The April 2025 survey conducted by the Annenberg Public Policy Center leverages a nationally representative panel, providing critical insights into current trends in public understanding and behavior around hypertension. Through such meticulous research, policymakers, healthcare providers, and communicators can tailor interventions that resonate with diverse populations, ensuring scientific advances translate into tangible health improvements. Awareness efforts targeting misperceptions hold promise in empowering individuals to take control of their cardiovascular health proactively.
Emerging data reinforce the notion that hypertension is not merely a medical diagnosis but a societal challenge requiring coordinated efforts spanning clinical care, community engagement, and health communication. As research continues to refine optimal blood pressure targets and treatment modalities, sustaining informed public dialogue is indispensable. When patients, providers, and the public collectively cultivate accurate knowledge and effective habits, the burden of hypertension-related diseases may finally begin to decline measurably.
In conclusion, high blood pressure persists as a silent but formidable threat to public health in America. While the foundational understanding of its management is present among many, critical gaps remain in defining what constitutes hypertension and recognizing its often invisible progression. Comprehensive education, widespread screening, and adherence support must converge to combat this epidemic. By bridging these divides, society can reduce preventable cardiovascular events and enhance the longevity and quality of life for millions.
Subject of Research: People
Article Title: Widespread Misconceptions and Behavioral Gaps Mark Public Understanding of High Blood Pressure, National Survey Finds
News Publication Date: April 2025
Web References:
- https://www.cdc.gov/high-blood-pressure/about/index.html
- https://www.annenbergpublicpolicycenter.org/wp-content/uploads/w24-pr-hbp-topline-2cat-v5.pdf
- https://newsroom.heart.org/news/high-blood-pressure-redefined-for-first-time-in-14-years-130-is-the-new-high
- https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings/monitoring-your-blood-pressure-at-home
References: See topline and methods report from Annenberg Public Policy Center (links above)
Image Credits: Annenberg Public Policy Center