Hepatocellular carcinoma (HCC) stands as one of the most formidable challenges in oncology today, representing about 90% of all primary liver cancers. This malignancy is notorious for its aggressive clinical behavior, high mortality rates, and overall poor prognosis. Despite notable advancements in surgical techniques, local regional therapies, targeted agents, and immunotherapies, the survival landscape for HCC patients has remained grim. This dismal outlook underscores the urgent need to dissect the intricate molecular mechanisms that fuel HCC progression, as well as to identify robust molecular biomarkers for early detection and prognostication. Such breakthroughs could pave the way for the development of superior therapeutic interventions.
A defining feature of HCC’s tumor microenvironment is hypoxia—the condition of low oxygen tension—which fundamentally alters cellular behavior and drives tumor progression. Central to the cellular adaptation to hypoxia is the hypoxia-inducible factor-1α (HIF-1α), a transcription factor that orchestrates the expression of a wide array of genes enabling tumor survival and growth under oxygen-deprived conditions. Normally, HIF-1α is tightly regulated and rapidly degraded via the Von Hippel-Lindau (VHL) tumor suppressor-mediated ubiquitin-proteasome pathway. However, in the context of HCC, aberrant stabilization and activation of HIF-1α are commonly observed in patients with poor outcomes. This irregular activation supports oncogenic processes such as angiogenesis, metabolic reprogramming, and metastatic dissemination, positioning HIF-1α as a critical therapeutic target.
Until recently, the precise molecular circuitry through which hypoxia drives HCC remained elusive. A groundbreaking collaborative effort spearheaded by Professors Dongsheng Huang, Qiuran Xu, Di Cui, and Kangsheng Tu has uncovered a novel and intricate regulatory mechanism involving the ubiquitin conjugation enzyme E2 variant 1 (UBE2V1). Their research reveals that UBE2V1 forms a self-propagating positive feedback loop with HIF-1α, significantly amplifying oncogenic signaling and fostering HCC progression. This discovery not only sheds light on the complexity of hypoxia signaling but also opens a promising avenue for targeted interventions.
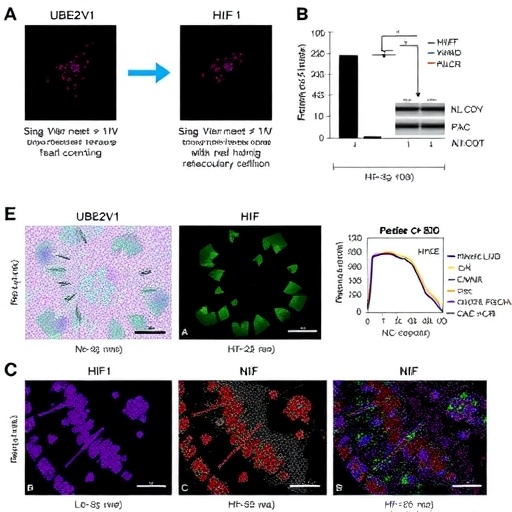
Through meticulous molecular analysis, the team identified UBE2V1 as a hypoxia-responsive gene directly transcriptionally activated by HIF-1α. Mechanistically, HIF-1α binds to a specific hypoxia-response element located between positions −208 and −201 base pairs on the UBE2V1 promoter, thus upregulating its expression. The clinical significance of this activation is profound; UBE2V1 is frequently overexpressed in HCC tumor samples, correlating strongly with advanced tumor stages and poor patient prognoses. Functionally, elevated UBE2V1 levels were shown to promote the proliferation and migratory capabilities of HCC cells, hallmark traits of malignant tumor progression.
Delving deeper into the molecular interactions, the researchers uncovered that UBE2V1 competes with HIF-1α for binding to the β-domain of the VHL protein. Critically, when complexed with ubiquitin-conjugating enzyme UBE2S, UBE2V1 catalyzes K11/K48-linked polyubiquitination at lysine 196 on VHL itself, earmarking VHL for proteasomal degradation. This targeting of VHL compromises its ability to ubiquitinate HIF-1α, consequently reducing HIF-1α’s degradation. The resulting accumulation of stabilized HIF-1α leads to its enhanced translocation into the nucleus and potentiation of transcriptional activity, thereby creating a self-sustaining loop that exacerbates the hypoxic tumor microenvironment.
This elegant but pernicious feedback mechanism ensures persistent activation of hypoxia signaling, mounting a continuous threat by supporting angiogenic factors and metabolic adaptations conducive to tumor growth and metastasis. The clinical implications are compelling: disrupting this axis holds the promise to significantly impede HCC tumorigenesis. Experimental knockdown of UBE2V1 or pharmacological inhibition of HIF-1α in vivo demonstrated marked suppression of tumor growth and metastatic spread, reinforcing the potential therapeutic value of targeting the UBE2V1-HIF-1α loop.
Beyond its implications in HCC biology, this study enriches the broader understanding of ubiquitin-proteasome system dysregulation in cancer. By highlighting a unique mechanism wherein an E2 variant subverts the canonical pathway to stabilize an oncogenic transcription factor, it prompts reconsideration of ubiquitination targets and regulators as fertile ground for anti-cancer drug discovery. Importantly, the specificity of UBE2V1 interaction with VHL suggests a novel molecular vulnerability that could be exploited with targeted inhibitors designed to disrupt this feedback loop.
Looking forward, integration of this molecular insight into translational and clinical research is paramount. Stratifying HCC patients based on UBE2V1 expression or activity could sharpen prognostic accuracy and tailor therapeutic regimens. Additionally, combinatorial therapies pairing existing HIF-1α inhibitors with agents targeting UBE2V1-mediated ubiquitination may yield synergistic effects. Equally important will be evaluating the potential off-target impacts and toxicity profiles of such approaches to ensure patient safety and maximize clinical benefit.
This pioneering work sets the stage for a new paradigm in combating one of the most lethal malignancies worldwide. UBE2V1 emerges not just as a molecular cog but as a master regulator sustaining hypoxia-induced oncogenesis in HCC via a positive feedback loop with HIF-1α. As research unfolds, this axis could revolutionize the molecular targeting strategies, offering hope where once there was despair in liver cancer therapy.
In summary, the elucidation of the UBE2V1-HIF-1α feedback loop provides a compelling mechanistic explanation for sustained hypoxia signaling in hepatocellular carcinoma, highlighting UBE2V1’s dual role as both a hypoxia-inducible gene and an active destabilizer of VHL. This mechanistic revelation opens exciting therapeutic vistas aimed at disrupting this oncogenic circuit to hinder HCC progression and improve patient survival outcomes. The road ahead involves validating this axis as a prognostic biomarker and developing precise inhibitors capable of breaking the vicious cycle of hypoxia-driven liver tumor growth.
Thus, this innovative study not only enhances the molecular narrative of HCC pathogenesis but also illuminates a promising beacon for future cancer biology and treatment research. As targeted therapies continue to evolve, pinpointing such molecular interactions and feedback loops will be instrumental in outmaneuvering cancer’s adaptive resilience and reshaping clinical outcomes.
Subject of Research: Not applicable
Article Title: UBE2V1 Promotes Hepatocellular Carcinoma Progression by Forming a Positive Feedback Loop with HIF-1α
News Publication Date: 23-Dec-2025
Web References: 10.34133/research.1041
Image Credits: Copyright © 2025 Zibo Yuan et al.
Keywords: Hepatocellular carcinoma, HCC, hypoxia, HIF-1α, UBE2V1, VHL, ubiquitination, tumor microenvironment, ubiquitin-proteasome pathway, cancer progression, molecular mechanisms, targeted therapy