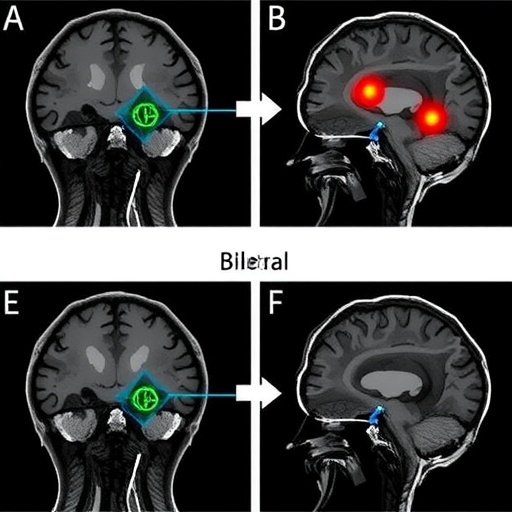
In the evolving landscape of Parkinson’s disease treatment, a recent study has illuminated critical differences in brain network activity depending on whether deep brain stimulation (DBS) is applied unilaterally or bilaterally to the subthalamic nucleus (STN). As the therapeutic use of STN-DBS becomes increasingly refined, understanding the precise neurofunctional impact of stimulation strategies remains essential to optimizing patient outcomes and minimizing adverse effects. The groundbreaking research spearheaded by Santyr, Boutet, Abbass, and colleagues offers unprecedented insights into these neurofunctional distinctions, shedding light on how unilateral and bilateral DBS engage complex brain circuits in varying patterns.
Deep brain stimulation has revolutionized treatment options for patients with Parkinson’s disease, particularly those experiencing motor fluctuations and medication-refractory symptoms. Traditionally, DBS involves the implantation of electrodes into targeted brain regions such as the STN to deliver electrical impulses that modulate aberrant neuronal activity. Clinically, bilateral STN-DBS—stimulating both hemispheres—is often preferred due to its robust effects on motor symptoms. However, debates have persisted regarding the differential neurophysiological consequences and functional connectivity outcomes produced by unilateral versus bilateral stimulation paradigms, with significant implications for therapy customization.
The study in question employed state-of-the-art neuroimaging and functional network analysis tools to explore these differences with unmatched granularity. By harnessing resting-state functional MRI alongside advanced graph theory metrics, the researchers mapped and compared whole-brain connectivity patterns in patients receiving unilateral versus bilateral STN-DBS. This approach enabled the team to parse out not only local effects at the stimulation sites but also remote influences reflected in large-scale brain networks critical for motor control, cognitive processes, and sensorimotor integration.
One of the landmark findings from the analysis is the pronounced modulation of functional networks implicated in motor and cognitive domains that vary based on the laterality of stimulation. Bilateral STN-DBS led to widespread, bilateral changes in connectivity within sensorimotor circuits, aligning with its demonstrated efficacy in suppressing cardinal motor symptoms like bradykinesia and rigidity. In contrast, unilateral DBS produced more localized connectivity enhancements, predominantly affecting networks contralateral to the side of stimulation. This pattern suggests a more circumscribed neuromodulatory effect potentially coupled with reduced side effects, illuminating a nuanced trade-off between therapeutic breadth and specificity.
Delving deeper into the network dynamics, the study revealed significant alterations in the basal ganglia-thalamocortical loops integral to movement regulation. Bilateral stimulation induced a recalibration of these loops, resulting in enhanced functional integration and synchronization across hemispheres. These changes likely reflect the restoration of more balanced activity within these loops that Parkinson’s disease pathophysiology disrupts. Unilateral stimulation, by contrast, appeared to modulate these circuits asymmetrically, achieving partial normalization with a different profile of network engagement.
Remarkably, cognitive and associative networks also exhibited distinct responses contingent upon stimulation laterality. The bilateral DBS cohort showed modifications in prefrontal and parietal networks, which could influence executive functions and attentional processes. This finding aligns with occasional clinical observations of cognitive side effects following bilateral STN-DBS, underscoring the need for neurofunctional monitoring and tailoring of stimulation parameters. Unilateral stimulation’s impact on these networks was more restrained, potentially offering a favorable cognitive safety profile that merits further exploration.
A particularly innovative aspect of the study lies in its use of network topology measures such as degree centrality and clustering coefficients. These quantifications provided objective markers of how nodes within the brain’s functional architecture reorganize with electrical stimulation. Bilateral stimulation tended to increase global efficiency and network integration, supporting the concept of enhanced communication across disparate brain regions. Conversely, unilateral stimulation maintained higher modularity, preserving more distinct network communities, which may correspond to differential clinical outcomes.
Furthermore, the analysis of interhemispheric connectivity exposed subtle but significant dissimilarities. Bilateral STN-DBS promoted stronger homotopic functional coupling between hemispheres, potentially restoring symmetry disrupted in Parkinson’s disease. Unilateral stimulation did not elicit this effect to the same extent, emphasizing how laterality of electrode placement influences not only local but also remote neurophysiological processes. These nuances highlight the complexity of DBS mechanisms beyond simple linear models of stimulation effects.
The temporal dynamics of DBS-induced network changes also emerged as a critical consideration. The study suggested that the onset and durability of network reorganization differ between unilateral and bilateral stimulation. Bilateral DBS seemed to accomplish rapid and sustained network integration shifts, whereas unilateral DBS brought about more gradual or transient effects. This temporal dimension may relate to variability in clinical symptom relief trajectories and informs strategies for programming and longitudinal monitoring.
This research holds profound clinical implications for personalized medicine in Parkinson’s disease management. The capacity to predict how unilateral versus bilateral stimulation will modulate an individual’s functional brain networks opens avenues for tailoring DBS approaches that maximize benefit while minimizing cognitive and neuropsychiatric side effects. Particularly for patients with asymmetric symptom profiles or cognitive vulnerabilities, unilateral STN-DBS might represent a balanced compromise pending corroborative studies.
Importantly, the findings challenge the conventional notion that bilateral stimulation is invariably superior, suggesting that the choice of unilateral versus bilateral STN-DBS should consider detailed functional network consequences beyond symptomatic profiles alone. This study provides a compelling argument for integrating multimodal neuroimaging and network neuroscience techniques into clinical decision-making frameworks for DBS therapy customization.
The authors acknowledge certain limitations, including sample size and inter-individual variability, which warrant cautious extrapolation. They advocate for longitudinal and larger cohort studies integrating clinical, neuroimaging, and electrophysiological data to further unravel the multifaceted neurobiology underlying DBS effects. Future work could also explore how stimulation parameters—pulse width, frequency, amplitude—influence functional network modifiability.
In sum, this pivotal study enriches our understanding of the brain-wide network effects elicited by unilateral and bilateral deep brain stimulation of the subthalamic nucleus. It delineates fundamental differences in functional connectivity profiles that underpin the disparate clinical outcomes observed with these approaches. By leveraging the tools of network neuroscience and advanced neuroimaging, it paints a more sophisticated picture of DBS as not merely a focal intervention but a broad modulator of distributed brain systems.
As DBS technologies evolve—encompassing adaptive stimulation and closed-loop paradigms—such mechanistic insights become indispensable. They enable clinicians and researchers to refine stimulation strategies informed by objective biomarkers of brain function. Consequently, this work sets the stage for accelerating the transition toward truly personalized neuromodulation therapies that optimize both motor and cognitive outcomes for individuals with Parkinson’s disease.
Ultimately, this research underscores that the future of DBS lies in harnessing the brain’s intrinsic connectivity architecture. Understanding how unilateral and bilateral stimulation differentially recalibrate these dynamic networks will catalyze innovations that enhance therapeutic precision and patient quality of life. This landmark contribution represents a paradigm shift in how we conceptualize and implement deep brain stimulation interventions for neurodegenerative disorders.
Subject of Research: Functional network differences induced by unilateral versus bilateral deep brain stimulation of the subthalamic nucleus in Parkinson’s disease patients.
Article Title: Functional network differences between unilateral and bilateral deep brain stimulation of the subthalamic nucleus.
Article References:
Santyr, B., Boutet, A., Abbass, M. et al. Functional network differences between unilateral and bilateral deep brain stimulation of the subthalamic nucleus. npj Parkinsons Dis. 11, 215 (2025). https://doi.org/10.1038/s41531-025-01064-2
Image Credits: AI Generated